Understanding Bronchial Cells: Key to Respiratory Health


Intro
Bronchial cells play a crucial role in the respiratory system. They are part of the bronchial epithelium, which lines the airways and is essential for proper lung function. These cells not only create a barrier against pathogens and particulates but also produce mucus, facilitate immune responses, and help in maintaining the overall health of the respiratory tract.
Understanding the specific functions and types of bronchial cells can lead to better insights into respiratory health and diseases. Their interaction with environmental factors, such as pollutants and allergens, can significantly impact their function.
This article seeks to address the complexity of bronchial cells, summarizing their structural composition, types, and functions. The implications of dysfunction and the importance of current research trends will be discussed to highlight their significance in both normal physiology and pathological conditions.
Research Overview
Summary of Key Findings
Recent studies shed light on the various types of bronchial cells, each with distinct roles. For example, ciliated cells are pivotal for moving mucus out of the airways, while goblet cells are responsible for mucus production. Dysfunction in these cells can lead to respiratory ailments like asthma or chronic obstructive pulmonary disease (COPD). These findings emphasize the intricate balance needed for maintaining respiratory health.
Research Objectives and Hypotheses
The objectives of this research are to:
- Investigate the structural and functional roles of different types of bronchial cells.
- Assess the impact of environmental factors on bronchial cell health.
- Explore emerging therapeutic approaches targeting bronchial cell dysfunction.
The hypothesis suggests that bronchial cell health directly correlates with environmental exposure and overall respiratory wellbeing.
Methodology
Study Design and Approach
This study employs a multi-faceted approach, combining in vitro and in vivo methods to assess bronchial cell function under various conditions. Experimental designs include exposure to environmental stressors, long-term monitoring of cell health, and analysis of responses in controlled environments.
Data Collection Techniques
Data collection involves several techniques, such as:
- Histological analysis to observe the structural integrity of bronchial cells.
- Cytometric techniques for measuring cell activity.
- Molecular analysis to understand the pathways involved in bronchial cell responses.
By utilizing these methodologies, the research aims to provide comprehensive insights into the roles of bronchial cells and their implications for respiratory health.
Preamble to Bronchial Cells
Bronchial cells play a vital role in maintaining respiratory health. They form a protective barrier, contribute to mucociliary clearance, and are involved in immune responses. Understanding bronchial cells helps reveal how our body protects itself against diseases and environmental stressors. In this article, we will explore their structure, classification, and functions. We will also discuss how they react to various conditions and factors.
Definition and Classification
Bronchial cells are specialized epithelial cells located within the bronchial tree. They line the trachea, bronchi, and bronchioles, contributing to the airway's structure and function. The bronchial epithelium consists of various cell types, each contributing differently to respiratory health. The major types of bronchial cells include:
- Ciliated Cells: These cells help move mucus and trapped particles out of the airways. Their coordinated ciliary movement is crucial for the effective clearance of pathogens and debris.
- Secretory Cells: Goblet cells and submucosal glands fall under this category. They produce mucus, which traps foreign particles and microorganisms, aiding in their removal from the respiratory system.
- Basal Cells: These cells are progenitor cells capable of differentiating into other bronchial cell types. They play an important role in epithelium regeneration and repair, especially after injury.
Historical Perspective
The study of bronchial cells has evolved significantly over time. Initially, researchers focused primarily on understanding the anatomical structure of the respiratory system. As technology advanced, scientists began to explore the functions of individual cell types within the bronchial epithelium.
Early 20th-century histological techniques allowed for the identification of various cell types. Studies revealed how ciliated cells and secretory cells work together to maintain airway hygiene. In recent decades, advances in molecular biology and imaging techniques have deepened our understanding of how bronchial cells respond to environmental changes and infections. This progress has highlighted their importance in both health and disease.
Recognizing the multifaceted roles of bronchial cells is crucial for exploring therapeutic interventions for respiratory diseases. More research continues, focusing on understanding these cells' responses in pathological conditions and their potential role in regenerative medicine. This exploration is vital to developing targeted therapies that could enhance bronchial function and improve respiratory health.
Anatomy of the Bronchial Tree
The bronchial tree is divided into the main bronchi, secondary bronchi, and tertiary bronchi, eventually leading to smaller branches known as bronchioles. This division increases the surface area available for gas exchange and supports a complex network of bronchial cells, each with specific functions vital for maintaining respiratory health. Understanding this anatomy not only sheds light on the operational aspects of the respiratory system but also highlights how disruptions in this architecture can lead to respiratory diseases.
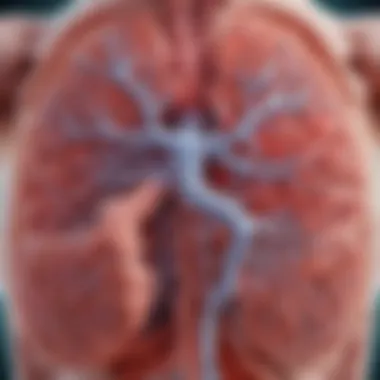

Structure of the Airway Epithelium
The airway epithelium is a critical component of the bronchial tree. It is primarily composed of a pseudostratified columnar epithelium featuring ciliated cells, goblet cells, and basal cells. This structure serves not only as a barrier but also plays a crucial role in the process of mucociliary clearance, preventing the accumulation of pathogens and particulate matter.
The presence of cilia on the surface of the epithelial cells is significant. These tiny, hair-like structures move in a coordinated fashion to transport mucus, which traps inhaled particles, up towards the throat. This mechanism is essential for keeping the airways clear and functions optimally when the integrity of the epithelial layer is intact. Damage to this epithelium can result in impaired clearance and increased susceptibility to infections.
Types of Bronchial Cells
Understanding the different types of bronchial cells is essential for grasping their unique contributions to respiratory health.
Ciliated Cells
Ciliated cells are characterized by the presence of cilia on their apical surface. These cells are primarily responsible for mucociliary clearance, an important function in protecting the airways. They help move mucus and trapped particles out of the respiratory system. This function is particularly beneficial in maintaining clear airways and reducing the risk of infections. A key characteristic of ciliated cells is their ability to rapidly sweep the mucus towards the pharynx. However, when ciliated cells are damaged by environmental factors such as pollution or smoking, their ability to clear mucus is compromised. This can lead to increased respiratory issues.
Secretory Cells
Secretory cells, including goblet cells and submucosal glands, play a vital role in producing mucus. This mucus serves to trap inhaled debris and protect underlying tissues from irritants. The production of mucus is a protective mechanism; it ensures that pathogens do not breach the airway epithelium. A key characteristic of secretory cells is their ability to increase mucus output in response to irritants, which is beneficial in keeping the airways moist and protected. However, overproduction can lead to blockages and contribute to conditions such as asthma and bronchitis.
Basal Cells
Basal cells are located at the base of the airway epithelium and serve as progenitor cells for other cell types. Their primary function is to help maintain epithelial integrity and facilitate regeneration after injury. A significant aspect of basal cells is their role in wound healing within the airway, which is crucial for restoring function after damage caused by infection or environmental exposure. Although basal cells are advantageous due to their regenerative capabilities, an overactive state may contribute to abnormal cell growth, potentially leading to conditions like dysplasia or cancer.
In summary, the anatomy and types of bronchial cells create a dynamic environment crucial for respiratory health. Understanding their structure and function provides insight into how they protect the airways and maintain homeostasis during health and disease.
Functions of Bronchial Cells
Understanding the functions of bronchial cells is essential in comprehending their role in respiratory health. Bronchial cells are primarily responsible for maintaining airway integrity and efficiency in gas exchange. Through their various functions, they contribute significantly to the respiratory system's overall functionality.
Mucociliary Clearance
Mucociliary clearance is a critical process facilitated by bronchial cells. The airway epithelium is lined with ciliated cells that work in tandem with mucus-secreting cells. These cilia beat in a coordinated manner, moving mucus loaded with particulate matter and pathogens out of the airways. This mechanism prevents the accumulation of harmful substances in the lungs and protects against infection. Dysfunction in this system can lead to various respiratory ailments, such as chronic bronchitis or asthma. To illustrate, in cases of cystic fibrosis, the ciliary action is impaired, leading to decreased mucus clearance, resulting in serious lung infections.
Barrier Function
The barrier function of bronchial cells is integral to preventing the entry of pathogens and pollutants into the lungs. The airway epithelium acts as a physical barrier that separates the internal environment from the external realities. Tight junctions between epithelial cells create a selective permeability barrier. This function is not only about physical obstruction but also supports ionic and fluid homeostasis. This barrier is essential for maintaining a healthy respiratory milieu, ensuring that necessary substances can pass while harmful agents are blocked out. An example of this is the impact of air pollution, which can compromise this barrier and lead to increased respiratory diseases.
Immune Modulation
Bronchial cells play a vital role in the immune modulation of the lungs. They can sense pathogens and initiate an immune response. This capability is crucial for responding to infections and allergens. The cells secrete various cytokines and chemokines, which recruit immune cells to infection sites, amplifying the body's defensive responses. A study has demonstrated that these bronchial cells can differentiate between harmless allergens and harmful pathogens, adjusting their responses accordingly. This differentiation is essential to avoid overreacting to non-threatening substances, reducing unnecessary inflammation.
"Bronchial cells are not just passive components of the airway; they are active players in maintaining respiratory health through mucociliary clearance, barrier function, and immune modulation."
Bronchial Cells in Health and Disease
Understanding the role of bronchial cells in health and disease is key for several reasons. Firstly, these cells are crucial for maintaining airway homeostasis. Their proper function ensures efficient gas exchange and facilitates immune responses. Abnormalities in bronchial cell function can lead to severe respiratory conditions that negatively impact overall health and quality of life.
Moreover, bronchial cells interact closely with various pathogens, allergens, and irritants in the environment. This interaction can trigger inflammatory responses, leading to both acute and chronic respiratory ailments. Overall, studying bronchial cells in this context provides insights into the mechanisms underlying respiratory diseases and helps identify potential targets for therapeutic intervention.
Impact of Infections
Viral Infections
Viral infections are a major aspect impacting bronchial health. Respiratory viruses, such as influenza and coronaviruses, can cause significant damage to bronchial epithelial cells. These viruses disrupt the barrier function and initiate inflammatory responses, which can hinder normal respiratory function. The ability of viruses to replicate within these cells can lead to increased cell death and a breakdown of mucociliary clearance.
Highlighting the capacity of viral infections to provoke robust immune responses is essential. This response, while protective, can sometimes cause excessive inflammation, contributing to symptoms like cough and wheezing. The unique feature of viral infections is their ability to alter bronchial cell function rapidly, leading to acute respiratory symptoms that require prompt medical attention.
Bacterial Infections

Bacterial infections also play a critical role in bronchial cell pathology. Pathogens like Streptococcus pneumoniae have a direct effect on bronchial epithelial integrity. They can induce apoptosis in bronchial cells and disrupt the protective mucin layer, leading to impaired respiratory defenses.
The key characteristic of bacterial infections is their potential for chronic colonization, often seen in conditions like chronic bronchitis. This persistent presence of bacteria can exacerbate inflammation, leading to a vicious cycle of recruitment of immune cells and ongoing damage to bronchial tissues. The unique feature of bacterial infections is their ability to form biofilms, aiding survival and complicating treatment options.
Allergic Reactions
Allergic reactions are another critical factor affecting bronchial cells. Allergens can incite an immune response, resulting in inflammation in the bronchial epithelium. This inflammation can lead to symptoms such as bronchospasm and increased mucus production. The interplay between bronchial cells and allergens influences the severity of conditions like allergic rhinitis and asthma.
Understanding how bronchial cells respond to allergens is vital. It provides insights into mechanisms of hypersensitivity, which can lead to targeted therapies. Notably, the release of mediators like histamines and cytokines during allergic responses contributes to the bronchial cell dysfunction and exacerbates respiratory symptoms.
Chronic Diseases
Asthma
Asthma is characterized by chronic inflammation of the airways, greatly influenced by bronchial cell behavior. The presence of eosinophils in the bronchial tissues indicates an ongoing allergic response. In asthma, bronchial cells exhibit altered functionality, contributing to hyperreactivity and airway remodeling.
The unique feature of asthma is its variable nature, where symptoms can be triggered by different environmental factors. Understanding bronchial cell responses in asthma can help identify precision treatments targeting specific inflammatory pathways.
Chronic Obstructive Pulmonary Disease (COPD)
Chronic Obstructive Pulmonary Disease is explicitly linked to long-term damage and inflammation of bronchial cells, often due to smoking. The hallmark of COPD is the loss of ciliated cells and increased secretory cell production, resulting in mucus hypersecretion.
The key characteristic of COPD is its progressive nature, leading to airflow limitation. The unique aspect of the disease is its association with significant morbidity and mortality. Studying bronchial cells in this context is essential for understanding disease mechanisms and developing effective therapeutic strategies.
In summary, bronchial cells are central to respiratory health and disease. Understanding their responses to infections, allergens, and chronic diseases helps to unravel the complexities involved in respiratory pathologies.
Environmental Influences on Bronchial Cells
Understanding environmental influences on bronchial cells is crucial for several reasons. The health of these cells significantly affects the overall respiratory system. Environmental factors such as air pollution and smoking can lead to cell dysfunction. This dysfunction contributes to various respiratory diseases. Recognizing these effects helps in creating effective preventive strategies and treatments.
Air Pollution
Air pollution is a major factor that impacts bronchial cells. Particulate matter, ozone, and other pollutants can penetrate the airways. They irritate the epithelial surface, leading to inflammation. Long-term exposure can result in chronic conditions, such as asthma and COPD. The bronchial epithelium serves as the first line of defense; thus, it is particularly vulnerable.
Importantly, air pollution alters the composition of bronchial secretions. This affects mucociliary clearance, making it harder for the body to expel pathogens and irritants. Research has shown correlations between polluted environments and increased rates of respiratory diseases.
Key points regarding air pollution impact on bronchial cells include:
- Inflammatory response: Increased inflammatory markers in response to pollutants.
- Mucus overproduction: Excess mucus can lead to blockages and greater risk of infection.
- Altered cell proliferation: Pollution can trigger abnormal growth of bronchial cells, leading to dysplasia.
"Reduced air quality is not just a public health issue. It directly harms the cells responsible for our breathing."
Smoking and Other Exposures
Smoking remains one of the most prominent threats to bronchial cell integrity. The inhalation of smoke introduces numerous toxins directly into the airways. These toxins can damage cellular DNA and impair normal cell functions. Ciliated cells, crucial for mucociliary clearance, become impaired over time. This can lead to chronic bronchitis and emphysema, both associated with COPD.
Additionally, other exposures like occupational hazards and secondhand smoke also pose risks. Various chemicals found in industrial environments can lead to similar pathologies as smoking. The vulnerability of bronchial cells to these toxins cannot be overstated.
It's essential to consider the following aspects concerning smoking and other exposures:
- Chronic irritation: Long-term exposure results in sustained inflammation and damage.
- Cellular alteration: Changes in phenotype of bronchial cells can lead to malignancies.
- Reduced immune response: Smoking compromises the immune function of respiratory epithelium.
Research Trends in Bronchial Cell Studies
Understanding research trends in bronchial cell studies is crucial in the context of respiratory health. These trends shed light on the ongoing developments in the field and how they influence therapeutic strategies and patient care. As researchers delve into the intricacies of bronchial cells, their innovative approaches inform us about cellular behavior, regeneration processes, and responses to various stimuli. This knowledge is directly applicable to the management of respiratory diseases.
Recent literature emphasizes the need for innovative methodologies and technologies in the study of bronchial cells. By advancing cell culture techniques, researchers can better mimic in vivo conditions. This approach allows for more accurate simulations of cellular responses to external factors, such as pollutants and pathogens. Understanding how bronchial cells react in a controlled environment provides insight that translates into practical medical applications.

Additionally, bronchial cells play a significant role in various pathologies. Identifying trends in these studies helps researchers recognize how bronchial cells adapt in diseases. Significant focus also exists on how environmental influences affect these cells, which adds another layer to their functional understanding. With a clearer picture of what alters bronchial cell behavior, targeted therapies can be developed.
Advancements in Cell Culture Techniques
Advancements in cell culture techniques are critical for the exploration of bronchial cells. Traditional two-dimensional cultures have limitations. To overcome these, three-dimensional culture systems are gaining popularity. This allows researchers to create more physiologically relevant models. These systems can replicate the complex architecture of bronchial tissue. As a result, cells exhibit behaviors more similar to those found in the human body.
One notable advancement is the use of organoids. Organoids are miniaturized and simplified organs produced in vitro. They have the potential to revolutionize research on bronchial cells. They can exhibit characteristics of the tissue they model. This can help identify how drugs affect cells in real-world scenarios, making it possible to test new therapies more effectively. The complexity and interactions observed in organoids provide deeper insight into cellular behavior.
New technology also includes microfluidic devices. These devices enable researchers to study bronchial cells in a dynamic environment, simulating airflow and different pressures. This technology can mimic conditions such as asthma attacks or exposure to pollutants. This adds a new dimension to understanding how bronchial cells function and respond. Overall, these advancements promise more precise and reliable insights into bronchial cell biology.
Role of Stem Cells in Regeneration
The role of stem cells in regeneration is a compelling aspect of bronchial cell studies. Research indicates that stem cells hold the potential to repair damaged bronchial tissue. This is particularly relevant for conditions such as Chronic Obstructive Pulmonary Disease (COPD) and severe cases of asthma, where the bronchial epithelium may suffer significant harm.
Adult stem cells found in the airways may contribute to the regeneration process. These cells can differentiate into various cell types, supporting the restoration of normal tissue structure. Understanding the mechanisms of stem cell activation and differentiation in the bronchial tree is vital. It sheds light on how to harness these processes for therapeutic benefits.
Moreover, the potential for stem cell therapies represents an exciting frontier. Ongoing studies aim to refine methods for utilizing stem cells to promote tissue repair. By investigating signaling pathways and the microenvironment in which these cells operate, researchers are developing targeted strategies to enhance regeneration. Stem cell-based therapies could offer significant benefits for individuals with chronic lung diseases, improving their overall respiratory health.
The understanding of bronchial cell dynamics offers potent avenues for innovative therapeutic strategies in respiratory diseases.
Examine current studies to evaluate how these approaches evolve. Keeping track of these trends can lead to more effective treatment options and improved patient outcomes.
Implications for Therapeutic Approaches
Understanding the role and function of bronchial cells is crucial when considering therapeutic strategies for respiratory health. These cells are integral to the airway's structural integrity and immune responses, thus shaping how diseases manifest and progress. This has significant implications for treatment options. Targeting bronchial cell functions can lead to improved outcomes in conditions like asthma and chronic obstructive pulmonary disease (COPD).
Pharmacological interventions often focus on enhancing bronchial cell functions. For instance, treatments may aim to improve mucociliary clearance, which directly influences the body's ability to expel pathogens and debris from the airways. Therefore, understanding these cells helps identify the most effective drug targets, paving the way for novel treatments that address the underlying cellular dysfunction rather than merely alleviating symptoms.
Additionally, gene therapy presents an innovative approach by potentially correcting the defects at the cellular level. By modifying bronchial cells genetically, it may be possible to restore normal function, particularly for hereditary conditions affecting the lungs.
Thus, exploring therapeutic approaches tailored to bronchial cell dynamics contributes significantly to advancements in respiratory medicine.
Pharmacological Interventions
Pharmacological interventions for bronchial cells aim to enhance their defensive roles in the respiratory system. Key aspects include:
- Bronchodilators: These medications widen the airways, improving airflow in conditions like asthma and COPD. They target smooth muscle surrounding the bronchi, which can indirectly influence bronchial cells' function.
- Corticosteroids: By reducing inflammation in the airways, these drugs can help maintain bronchial cell integrity and function, fewer flare-ups occur, and overall lung health improves.
- Mucolytics: These are designed to decrease mucus viscosity, facilitating clearance and improving response from ciliated cells in the epithelium. This is especially important in chronic lung diseases where mucus buildup is a problem.
"Effectively targeting bronchial cell functions in therapy not only addresses symptoms but promotes long-term respiratory health."
Gene Therapy
Gene therapy holds promise for direct intervention at the cellular level. For bronchial cells, this could mean:
- Correcting Genetic Defects: For patients with genetic disorders affecting lung function, targeting defective genes in bronchial cells could offer a definitive treatment solution.
- Promoting Regeneration: By stimulating the repair mechanisms within bronchial cells, gene therapy may restore normal function after injury or disease.
- Enhancing Immune Responses: Gene therapy can be used to introduce new genetic material that boosts the immune function of bronchial cells, offering better defense against infections and pollutants.
As the field of gene therapy evolves, its application to bronchial cells could revolutionize treatments for various respiratory conditions, moving beyond symptom management to more comprehensive and lasting solutions.
Finale
In this article, the discussion around bronchial cells has revealed their vital role in maintaining respiratory health. Bronchial cells contribute to critical functions such as mucus production, ciliary movements, and immune responses. These processes are crucial for keeping the airways clear and protecting against harmful agents.
During our exploration, several key findings emerged.
Summary of Key Findings
- Bronchial cells are structurally diverse, comprising ciliated cells, secretory cells, and basal cells, each serving distinct functions.
- Mucociliary clearance is essential for trapping and expelling pathogens and debris from the respiratory tract.
- Disruption in the function of bronchial cells can lead to severe respiratory issues like asthma and COPD.
- Environmental factors, such as air pollution and smoking, directly impact bronchial cell health, which can further exacerbate existing diseases.
"Understanding the functions of bronchial cells is not only important for basic science but also for the development of therapeutic strategies."
Future Directions in Research
Future research in bronchial cell studies can significantly advance our understanding of respiratory diseases. Possible avenues include:
- Investigating the impact of novel environmental toxins on bronchial cell function.
- Developing targeted drug delivery systems that enhance the efficacy of treatments at the cellular level.
- Exploring the potential of stem cells in regenerating damaged bronchial tissues.
- Further examination of genetic predispositions to bronchial cell dysfunction will help tailor personalized therapies.















